Alehra simplifies the process of analyzing insurance remittance data.
- For Therapists, Psychologists, Pediatricians, Primary Care, and Speech Therapy Clinics
EDI Lens: Turn Complex 835 Remittance Files into Clear Revenue Intelligence
Insurance remittance files (EDI 835) contain critical payment information, but they are often difficult to read, analyze, or reconcile. Alehra EDI Lens transforms raw remittance files into structured analytics that help practices understand payments, denials, payer performance, and revenue trends.
Upload remittance file. Analyze payments. Recover lost revenue.
Feature Capabilities
EDI 835 File Upload and Processing
Alehra allows practices to upload EDI 835 remittance files directly into the system.
Revenue Analytics Dashboard
EDI Lens converts remittance data into actionable financial insights.
Denial Pattern Analysis
EDI Lens analyzes denial information embedded in remittance files to help practices identify recurring issues.
Claim Reconciliation
EDI Lens supports reconciliation between billed claims and remittance payments.
EDI File Viewer
Alehra includes a built-in EDI viewer that allows users to inspect remittance files in both raw and structured formats.
See Your Insurance Payments with Clarity
EDI Lens provides a visual dashboard that transforms complex EDI remittance files into clear analytics and structured insights. Practices can view payment performance, analyze denial patterns, reconcile claims, and inspect EDI files through a single interface.
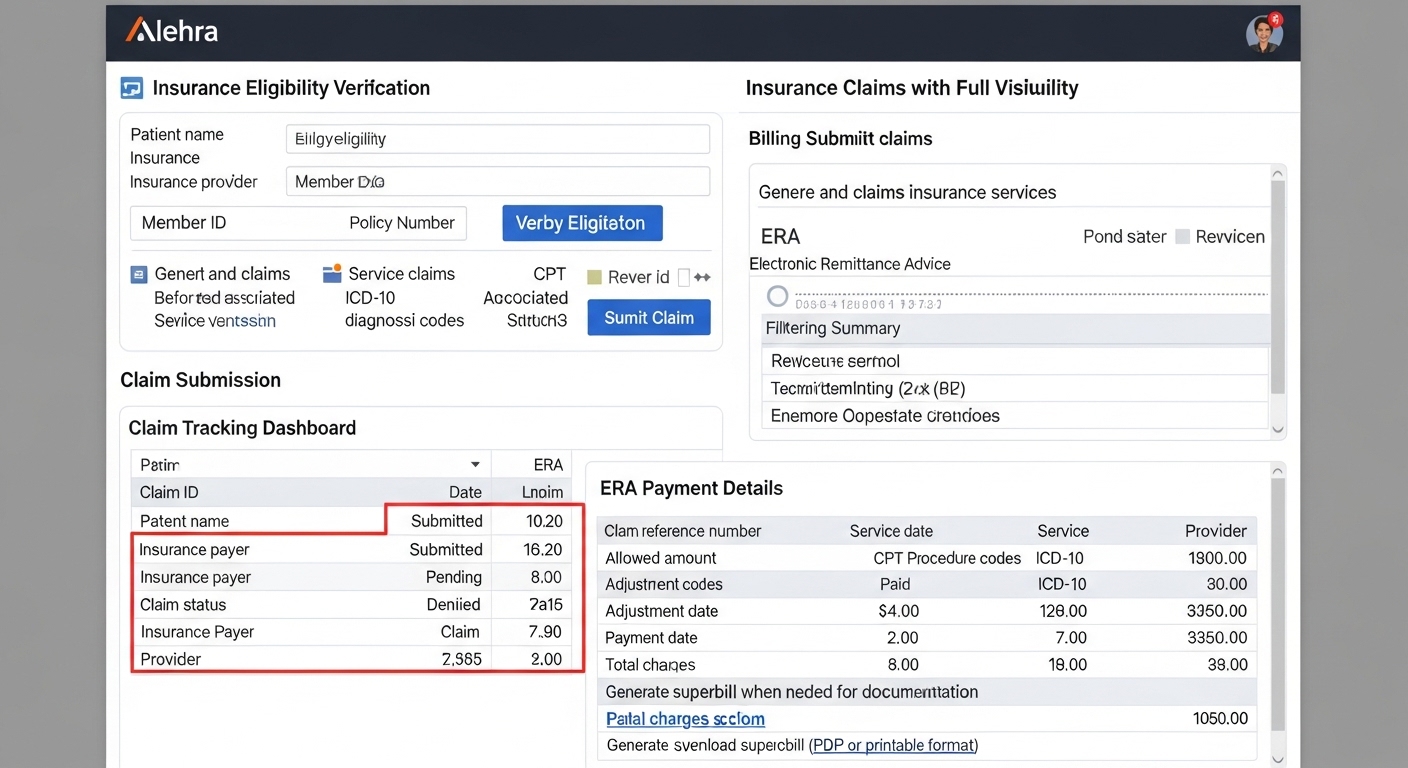
Improve Revenue Visibility and Recovery
Insurance remittance files contain valuable financial information, but most practices struggle to extract insights from them. EDI Lens transforms this data into meaningful analytics that support better revenue management.
Identify Revenue Loss
Practices can detect underpayments and denied claims that may otherwise go unnoticed.
Understand Denial Trends
Denial analysis helps billing teams identify recurring issues in claim submissions.
Improve Billing Decisions
Payer performance insights help practices understand how different insurance companies reimburse services.
Simplify Remittance Review
Structured views of EDI files make it easier to interpret remittance data without specialized EDI knowledge.
Connected to Alehra’s Billing and Claims Infrastructure
EDI Lens integrates directly with Alehra’s financial and billing workflows.
Insurance Billing & Claims
Reconcile remittance data with submitted claims
Payments Management
Track patient responsibility and received payments
Analytics Dashboard
Monitor financial performance across the practice
Provider Services
Analyze revenue by service and provider
From Remittance File to Revenue Insight
Upload EDI Remittance File
Billing teams upload EDI 835 remittance files into the system.
Automatic Data Parsing
Alehra extracts structured data including payments, claims, adjustments, and denial codes.
Analyze and Reconcile Payments
Practices review payment analytics, detect underpayments, and reconcile claims against remittance information.
Unlock Revenue Insights from Your Remittance Data
Alehra EDI Lens transforms complex insurance remittance files into clear analytics that help practices understand payments, denials, and reimbursement performance.
Turn raw EDI files into actionable revenue intelligence.
