AI Note Taking integrates directly with the Alehra clinical platform and documentation workflows.Captured notes can automatically connect to
- For Therapists, Psychologists, Pediatricians, Primary Care, and Speech Therapy Clinics
Revenue Automation: AI That Protects and Optimizes Your Revenue Cycle
Healthcare billing errors, coding inconsistencies, and claim submission issues can lead to costly denials and delayed reimbursements.
Smarter claims. Fewer denials. Stronger revenue performance.
Feature Capabilities
Automated Claim Scrubbing
Before claims are submitted, Alehra Revenue Automation analyzes billing data for potential issues.
AI-Powered Denial Prevention
The system continuously analyzes billing patterns and payer responses to identify scenarios that commonly result in denied claims.
Encounter Coding Insights
Alehra monitors clinical encounters to detect situations where billing codes may be under-coded or over-coded.
Reimbursement Pattern Monitoring
Revenue Automation analyzes reimbursement trends and payer behavior across submitted claims.
Configurable Guardrails and Approvals
Revenue Automation operates with configurable guardrails that allow practices to maintain oversight.
Revenue Automation Agent
The Revenue Automation dashboard allows administrators to enable AI agents that monitor billing workflows and optimize claim quality.
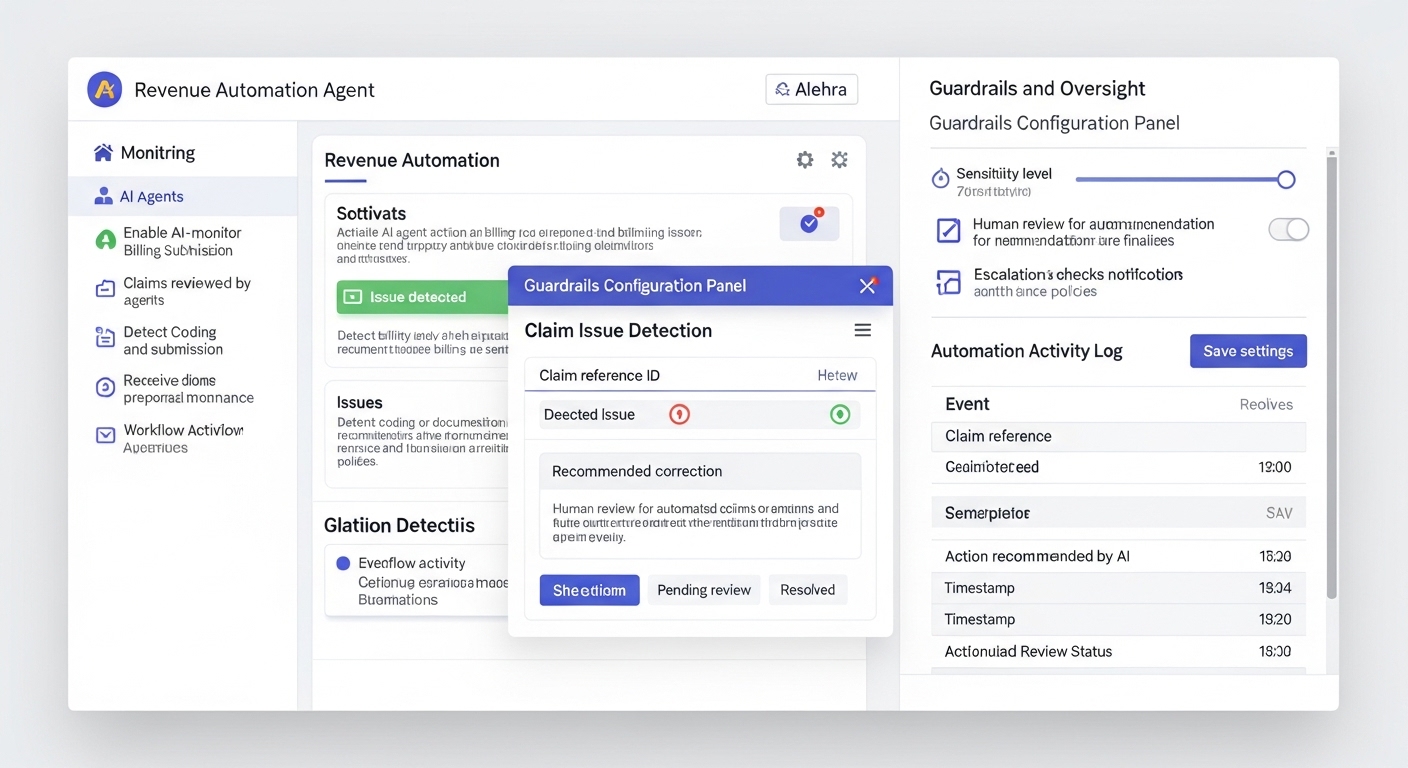
Revenue Automation Interface
The AI Note Taking interface operates seamlessly within the patient encounter workflow. Providers can capture the conversation, generate clinical notes, and review suggested documentation sections all within a single interface. This ensures that clinical information is organized, structured, and ready for
Billing Teams
Reduce claim errors and identify potential denials before submission.
Practice Administrators
Improve financial performance by detecting revenue leakage and optimizing claim accuracy.
Providers
Ensure documentation supports accurate coding and billing.
Healthcare Organizations
Increase clean claim rates and improve reimbursement outcomes.
Connected to Revenue Automation
Revenue Automation integrates across the Alehra revenue cycle ecosystem.
Insurance Billing & Claims
Reconcile remittance data with submitted claims
Payments Management
Track patient responsibility and received payments
Analytics Dashboard
Monitor financial performance across the practice
Provider Services
Analyze revenue by service and provider
Revenue Automation Steps
1. Encounter Documentation Is Completed
Providers complete clinical documentation during or after the patient visit.
2. Claims Are Prepared for Submission
Billing data is generated based on encounter documentation and coding.
3. AI Reviews the Claim
Alehra Revenue Automation analyzes the claim for coding issues, missing information, and denial risk indicators.
Strengthen Your Revenue Cycle With AI Automation
Alehra Revenue Automation helps practices detect billing risks early, reduce denials, and improve reimbursement outcomes.
Prevent revenue leakage and optimize your claims workflow.
