Alehra simplifies the process of analyzing insurance remittance data.
- For Therapists, Psychologists, Pediatricians, Primary Care, and Speech Therapy Clinics
Revenue Analytics: Turn Your Practice Data Into Financial Intelligence
Understanding the true financial health of a practice requires more than basic billing reports. Practices need clear insights into revenue trends, claim outcomes, payer behavior, and reimbursement performance.
Track performance. Improve collections. make data-driven financial decisions.
Feature Capabilities
Revenue Trend Tracking
The Revenue Analytics dashboard provides an instant overview of financial health across the practice.
Revenue Analytics Dashboard
Track revenue trends across months to identify growth patterns and financial fluctuations.
Payment Source Breakdown
Understanding where revenue comes from is critical for optimizing the revenue cycle.
Claims Processing Insights
Revenue Analytics tracks claims processing activity across the billing lifecycle.
Denial Analysis by Payer
Denials can significantly impact revenue. Alehra highlights denial patterns across different insurance payers.
Billing & Revenue Dashboard
The Revenue Analytics dashboard gives administrators and billing teams a clear visual overview of financial performance. Revenue trends, payment sources, claim outcomes, and denial patterns are presented through interactive visualizations that simplify complex financial data.
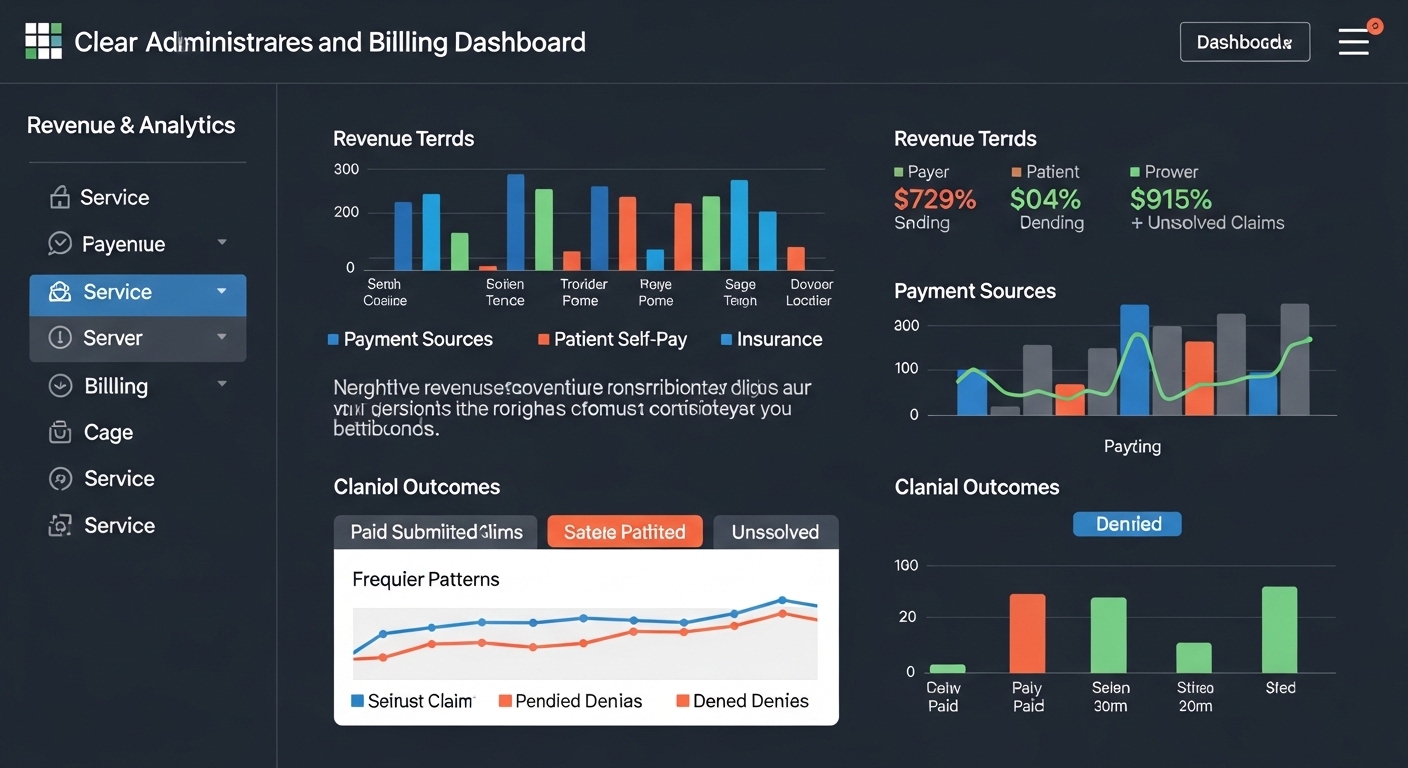
Improve Revenue Visibility and Recovery
Insurance remittance files contain valuable financial information, but most practices struggle to extract insights from them. EDI Lens transforms this data into meaningful analytics that support better revenue management.
Practice Owners
Gain full visibility into the financial performance of the practice and track revenue growth over time.
Billing Teams
Identify denial patterns and claim processing issues to improve reimbursement outcomes.
Operations Managers
Monitor key performance indicators such as claim approval rates, collection rates, and reimbursement timelines.
Financial Decision Makers
Use real-time analytics to identify revenue opportunities and optimize payer strategy.
Connected to Alehra’s Billing and Claims Infrastructure
EDI Lens integrates directly with Alehra’s financial and billing workflows.
Insurance Billing & Claims
Reconcile remittance data with submitted claims
Payments Management
Track patient responsibility and received payments
Analytics Dashboard
Monitor financial performance across the practice
Provider Services
Analyze revenue by service and provider
From Remittance File to Revenue Insight
Claims Are Submitted
Billing teams upload EDI 835 remittance files into the system.
Payments and Responses Are Recorded
Insurance payments, patient payments, and claim responses are automatically captured.
Financial Data Is Aggregated
Alehra processes revenue, billing, and claims data across the platform.
Turn Revenue Data Into Actionable Insights
Alehra Revenue Analytics helps practices move beyond basic billing reports and gain true financial visibility.
Monitor performance. Identify revenue opportunities. Optimize your revenue cycle.
