Alehra simplifies the insurance billing workflow for healthcare practices.
- For Therapists, Psychologists, Pediatricians, Primary Care, and Speech Therapy Clinics
Billing & Claims: Simplify Insurance Billing and Get Paid Faster
Insurance billing is one of the most complex parts of running a healthcare practice. Alehra simplifies this process by providing tools for insurance eligibility verification, claim generation, claim submission, claim tracking, and reimbursement reconciliation — all within a single platform.
Verify coverage. Submit claims. Track reimbursements.
Feature Capabilities
Insurance Eligibility Verification
Before providing care, practices can verify a patient’s insurance coverage directly within Alehra.
Automated Claim Generation
After services are delivered, Alehra automatically generates insurance claims using the billing and clinical information recorded during the visit.
Electronic Claim Submission
Alehra allows practices to submit claims electronically to insurance payers through its integrated claims infrastructure.
Claim Status Tracking
Alehra provides visibility into the status of submitted claims. Practices can track claims as they move through the billing lifecycle.
Electronic Remittance Advice (ERA)
Once an insurance payer processes a claim, Alehra retrieves the Electronic Remittance Advice (ERA) associated with the claim.
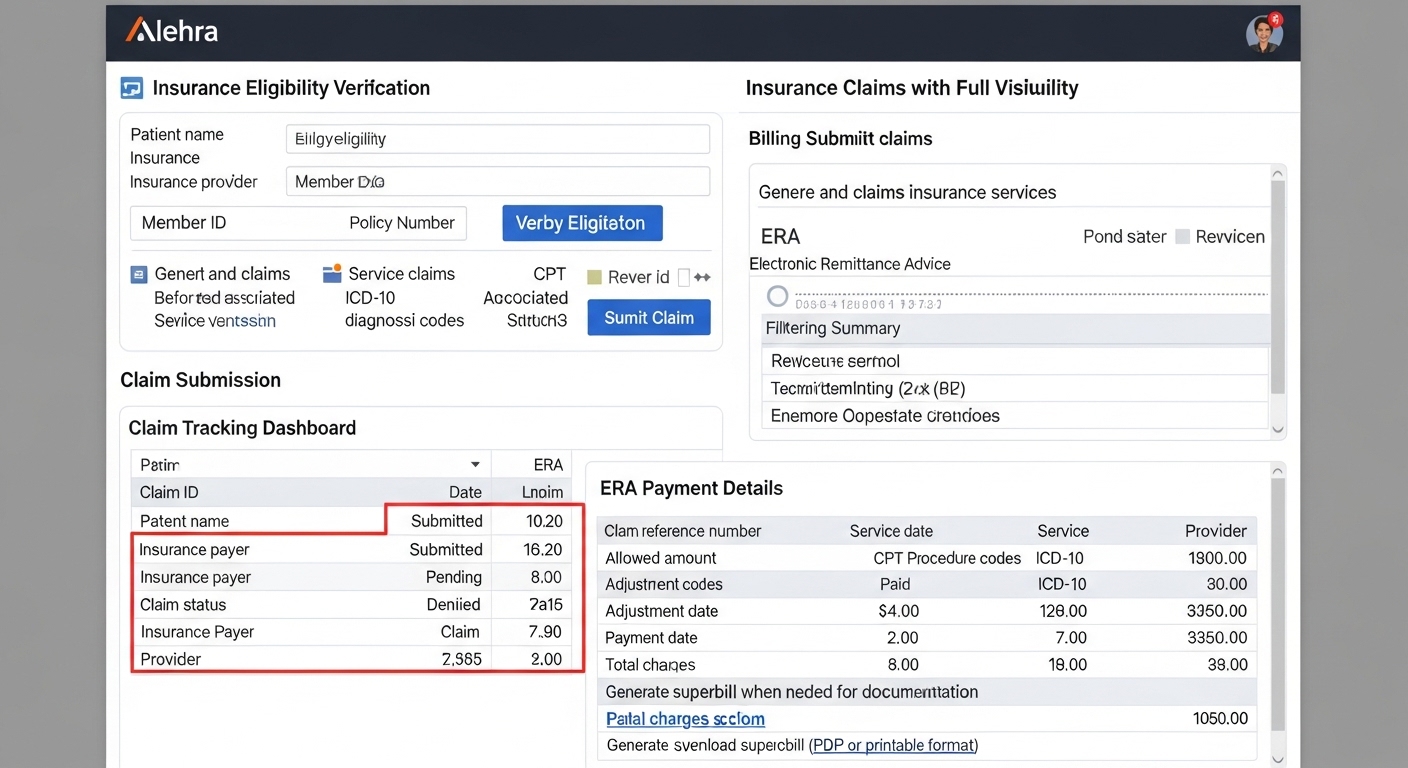
Manage Insurance Claims with Full Visibility
Alehra provides an intuitive interface where billing teams can verify eligibility, generate claims, monitor claim status, and review remittance information. The system allows staff to track insurance billing activity while maintaining visibility into service details and reimbursement outcomes.
Reduce Billing Complexity and Improve Revenue Cycle Efficiency
Insurance billing processes can become complicated when managed across multiple disconnected systems. Alehra simplifies these workflows and keeps billing information connected to patient care.
Reduce Claim Errors
Automated claim generation ensures claims include the required billing information and reduces manual mistakes.
Confirm Insurance Before Visits
Eligibility verification helps staff confirm coverage and patient responsibility before appointments.
Improve Billing Visibility
Billing teams can track claim progress and quickly identify rejected or denied claims.
Support Both Insurance and Private-Pay Models
Superbills allow practices to provide reimbursement documentation when operating outside insurance networks.
Connected to the Alehra Practice Platform
Claims tied to appointments and service dates
Scheduling
Payments linked to booked appointments
Providers Profiles
Provider credentials and NPI information used in claims
Payments
Patient responsibility balances managed through payment workflows
Client Notes
Diagnosis and procedure codes captured during visits
Client Portal
atients can access superbills and billing records
Insurance Billing in 3 steps
Verify Patient Eligibility
Before the visit, staff verify the patient’s insurance coverage and benefits.
Deliver Care and Generate Claim
Providers complete the session and the system generates a claim based on the services delivered.
Submit and Track Claim Status
The claim is submitted electronically and the billing team can track its status until payment is received.
Simplify Insurance Billing for Your Practice
Reduce billing complexity and improve your revenue cycle management.
Alehra helps practices verify insurance coverage, submit claims electronically, track claim status, and reconcile reimbursements — all from a single platform.
